A novel approach for improving the quality and deliverability of VMAT plans in head and neck cancer
Purpose/Objective
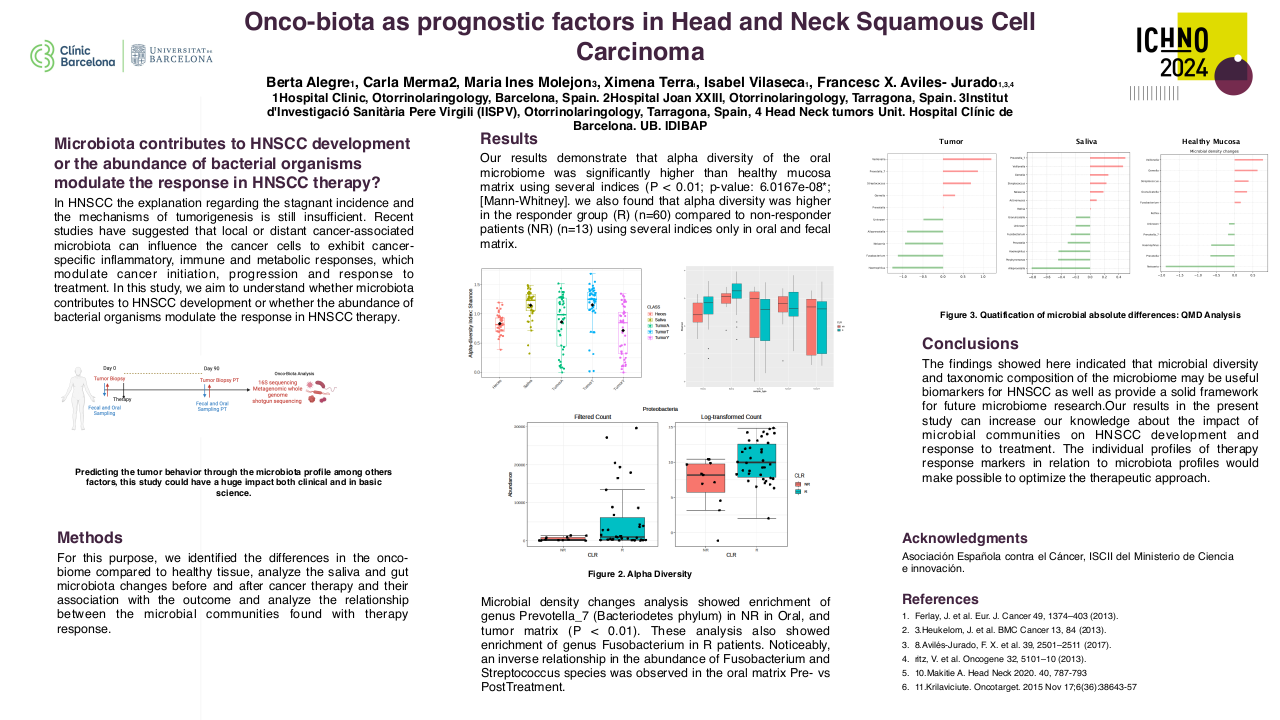
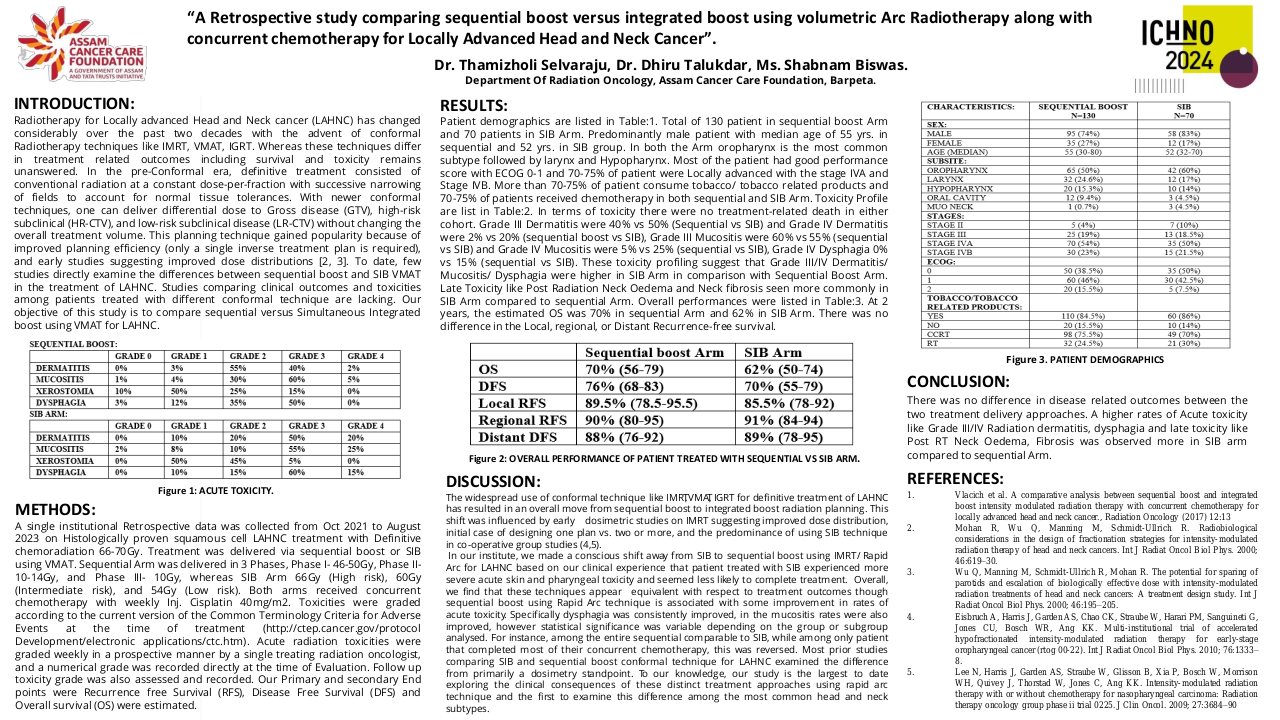
Advanced radiation techniques are frequently used in the treatment of squamous cell carcinoma of the head and neck (H&N). Volumetric modulated arc therapy (VMAT) is currently the standard treatment across the world. It provides good target volume coverage and enhanced conformal dose distributions while sparing the organs at risk (OARs). However, this may result in a considerable volume of low-dose region in the surrounding normal tissue. In the clinical practice, our oncology center has implemented the Triple Arc (TA) VMAT approach in head and neck cancer treatment planning using three full arcs to enhance the radiation outcomes and effectively spare midline structures. This dosimetric study was performed to verify Triple Arc Volumetric Modulated Arc Therapy (TA-VMAT) in head and neck cancer treatment planning using the simultaneous integrated boost (SIB) technique by proving its deliverability and dosimetric accuracy when compared to Dual Arc (DA)VMAT.
Material/Methods
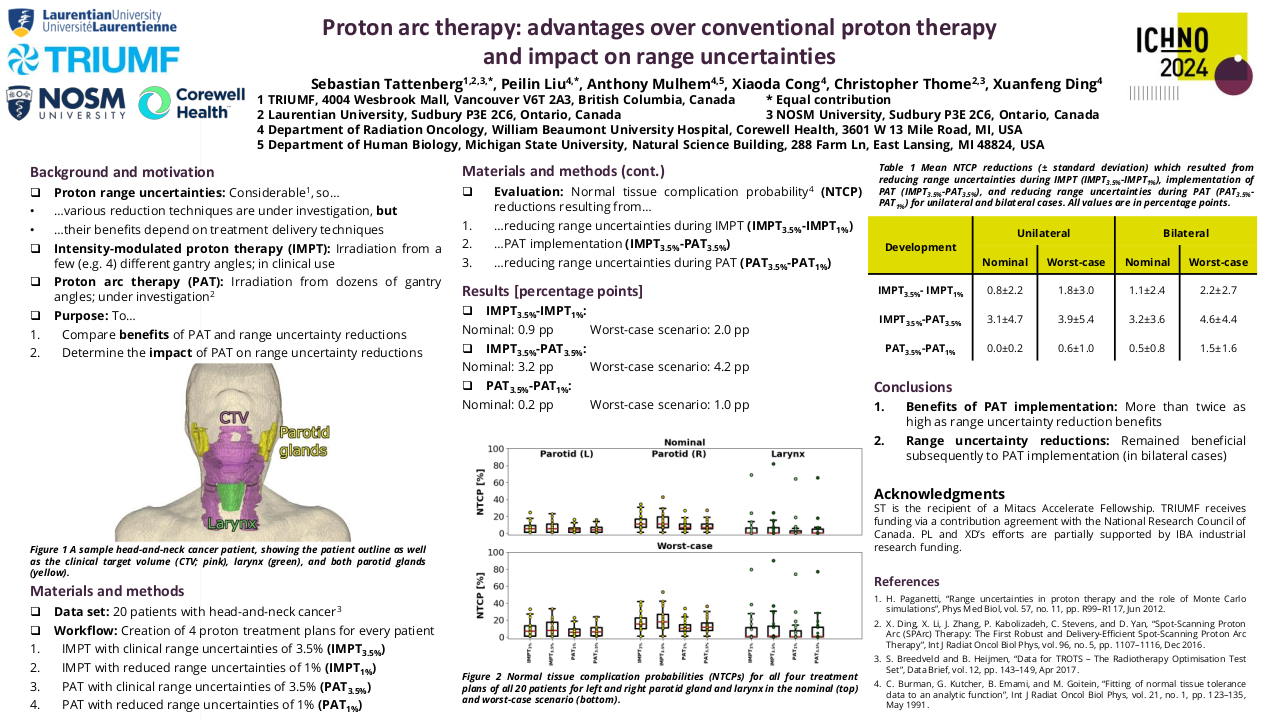
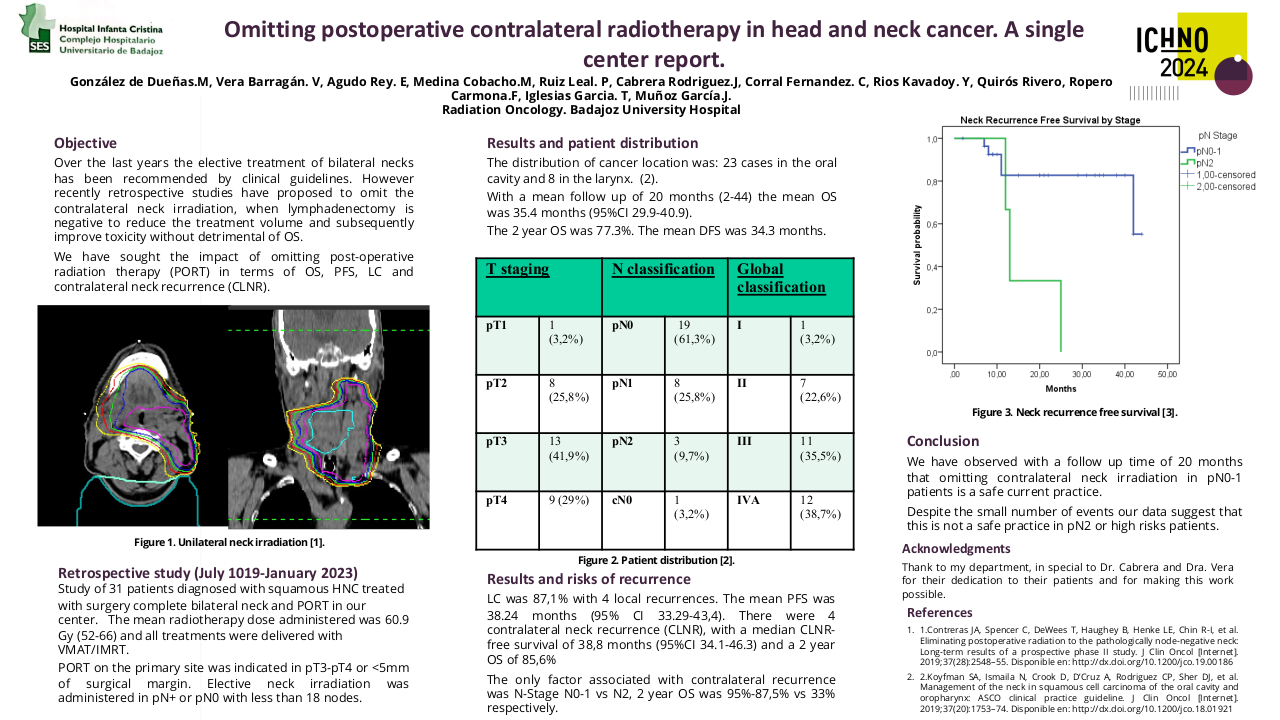
Thirteen head and neck cancer cases were randomly enrolled in this comparative study. The planning target volumes(PTVs) and OARs were defined using RTOG 0225/0615. Additionally, we identified the thyroid and trachea as well. For each case, two treatment plans TA and DA were generated by the Varian Eclipse planning system yielding a total of 26 treatment plans. Both plans have full arcs that span an angle between 179-181 CW and CCW using a collimator angle of 330 and 30 degrees for the CW, and CCW, respectively. However, in TA arc plans, a third arc with an 80-degree collimator angle was added. Doses of 70Gy, 63Gy, and 54 Gy were delivered to PTV high, intermediate, and low risk, respectively in 35 fractions using the SIB technique. All these treatment plans are assessed in terms of dosimetric quality, OARs sparing, and delivery efficiency.
Results
According to RTOG 0225/0615; both Triple Arc and Dual Arc plans provided appropriate target coverage while lowering OAR doses. However, TA-VMAT effectively managed the dose hotspot and maintained a consistent gantry speed for precise radiation delivery yielding a significantly enhanced target homogeneity and dose conformity in comparison to DA-VMAT ( P=0.02 and 0.002 respectively). Moreover, it provides superior dosage reduction to the brain stem, larynx, esophagus, trachea, and spinal cord. A paired-sample t-test was conducted to assess the value of using Triple-arc VMAT over Dual-arc VMAT in terms of the dose coverage, conformity index(CI), and homogeneity index(HI) for targets as well as the mean and maximum dosage for OARs. Treatment delivery time (min), monitor units (MUs) per fraction, and normal tissue integral dose(NTID) were also evaluated. The maximum dosage (Dmax) to the brain stem in TA-VMAT was significantly lower than in DA-VMAT (p=0.001). The spinal cord maximum dosage (Dmax) was significantly low in TA-VMAT as compared with DA-VMAT (p=0.002).TA-VMAT produced a significantly lower mean dose to the larynx (p=0.027) than DA-VMAT. The mean doses to the esophagus and trachea were significantly lower in TA than in DA treatment plans(p=0.008 and 0.001 respectively). Both treatment plans had almost the same mean treatment delivery time. There were no significant changes in the number of monitor units MU/ fraction or normal tissues integral dose NTID(p=0.057). These results suggest that the Triple Arc VMAT approach is unique, precise, and highly effective in reducing the dose of the OARs during radiation therapy among head and neck cancer patients.
Conclusion
In terms of target coverage and OAR sparing, radiation therapy treatment planning using TA-VMAT outperformed DA-VMAT, resulting in superior treatment outcomes without compromising delivery efficiency in patients with head and neck cancer. It has the potential to be a very effective, and high-quality radiation therapy approach.
1. Lee, N, Harris, J, Garden, AS et al. Intensity-modulated radiation therapy with or without chemotherapy for nasopharyngeal carcinoma: radiation therapy oncology group phase II trial 0225. J Clin Oncol 2009; 27: 3684–3690.CrossRefGoogle ScholarPubMed2. Lee, NY, Zhang, Q, Pfister, DG et al. Addition of bevacizumab to standard chemoradiation for locoregionally advanced nasopharyngeal carcinoma (RTOG 0615): a phase 2 multi-institutional trial. Lancet Oncol 2012; 13: 172–180.CrossRefGoogle ScholarPubMed3. White, P, Chan, KC, Cheng, KW, et al. Volumetric intensity-modulated arc therapy vs conventional intensity-modulated radiation therapy in nasopharyngeal carcinoma: a dosimetric study. J Radiat Res 2013; 54: 532–545.CrossRefGoogle ScholarPubMed4. Lee, TF, Ting, HM, Chao, PJ, Fang, FM. Dual arc volumetric-modulated arc radiotherapy (VMAT) of nasopharyngeal carcinomas: a simultaneous integrated boost treatment plan comparison with intensity-modulated radiotherapies and single arc VMAT. Clin Oncol (R Coll Radiol) 2012; 24: 196–207.CrossRefGoogle ScholarPubMed5. Wagner, D, Christiansen, H, Wolff, H, Vorwerk, H. Radiotherapy of malignant gliomas: comparison of volumetric single arc technique (RapidArc), dynamic intensity-modulated technique and 3D conformal technique. Radiother Oncol 2009; 93: 593–596.CrossRefGoogle Scholar6. Wolff, D, Stieler, F, Welzel, G et al. Volumetric modulated arc therapy (VMAT) vs. serial tomotherapy, step-and-shoot IMRT, and 3D-conformal RT for the treatment of prostate cancer. Radiother Oncol 2009; 93: 226–233.CrossRefGoogle ScholarPubMed